The Post Pandemic Practice: The Opportunity for Building Practice Resilience

The Post Pandemic Practice
The Opportunity for Building Practice Resilience is Now
Things have been pretty tough for medical practices lately. In 2020, profitable practices saw the impact of an over-dependence on volume-based reimbursements when patient volume and cash flow dropped to zero overnight.
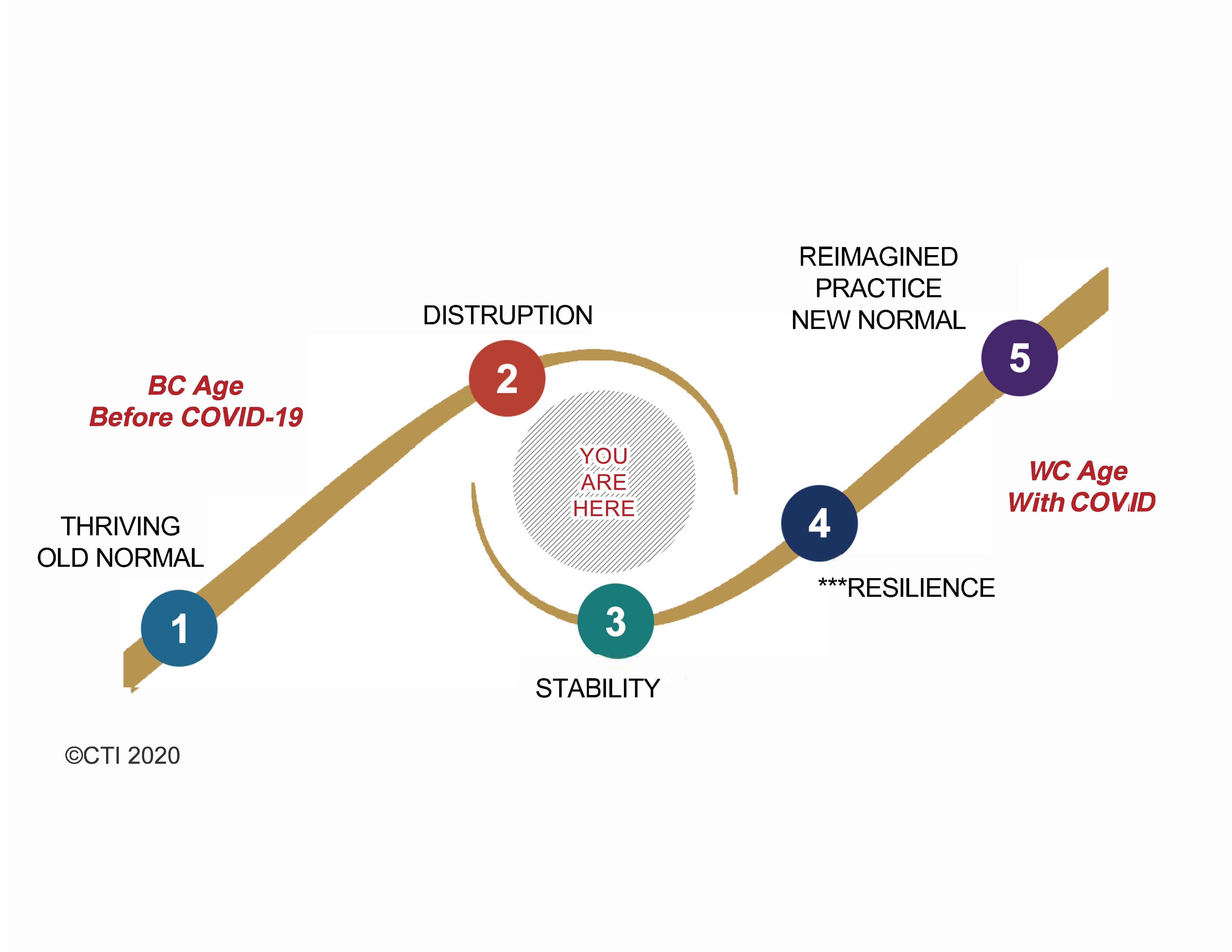
But what exactly does “stability and normalcy” really mean for medical practices in a post-pandemic world? Of course, it’s essential to stop the hemorrhaging, and getting patients through the door will certainly get practices moving again.
Yet is this enough? Will we be ok for the next unexpected event? Are we returning to a way of operating in a world where expectations have changed permanently, “skating to where the puck has been” rather than where it’s going to be?
While we seek “stability and normalcy,” we have an opportunity to build-in resilience in our clinical and business models. And if we do it right, we can develop a strong competitive advantage. Just as we diversify our investment portfolios, rebalancing at times of market extremes, this is the time for diversification in our business models to create better access and less dependency on volume alone. These questions can help you strategize:

Value-based care can mean vastly different things to different audiences, but the essential component is that reimbursement is somehow tied to the perceived value of services provided (quality, affordability, etc.). On one end of the spectrum, a value-based arrangement may look a lot like pure fee-for-service with a quality incentive tied to it. On the other end of the spectrum, this could mean a capitated model in which the group receives a monthly payment for each member. And in the middle are a variety of shared-savings models or models involving limited risk. The type of model that’s right for your situation depends on (1) your current environment, (2) the specific revenue challenges you are facing, and most importantly, (3) your capabilities as an organization. It also has implications on your balance of primary care versus specialist service line mix. We know this journey can be complicated, but in our experience helping clients identify the right play in this space, it’s not impossible.

In our work, we hear stories of leaders jumping to solutions (e.g., “We need to move more rapidly to value-based care!” or “We have to double-down on telehealth!” or “We need to further cut overhead!”). Taking some time to truly sense, reflect, and understand what’s going on in this emerging environment is an important first step in defining the problem at hand. Without this step, it’s possible to invest in solutions that miss the underlying issues. In some cases, we’re seeing that the real issue at hand is a lack of diversification in revenue sources (fee-for-service, value-based, and risk-based arrangements), payer mix, or even specialty mix. In other cases, it has to do with in-person and virtual access points. Don’t jump to solutions before ensuring your team is aligned on the specific problem you’re trying to solve.

Our understanding of what patients wanted during the pandemic may be different from what they want or expect now. For example, the rate of acceptance of telehealth options, particularly among seniors, has changed significantly. What role will this play as we move out of crisis mode, and how will it integrate into existing models of care? These are question that will require groups to re-examine their model of care and how it’s organized and delivered (and if it doesn’t exist, to define one) and to integrate these tools to support the model as opposed to being a standalone offering that may not necessarily drive value in the way we hope. It’s our experience that listening at these crucial inflection points, both to customers and to our caregivers, will be the key to success.

Expanding the role of scribes to help with care coordination, outreach, and closing care gaps is a relatively untapped opportunity that can lower costs and improve outcomes, not to mention physician well-being. Telemedicine, thoughtfully integrated into a care model, can expand capabilities and reach across a medical group, supporting specialists, behavioral health providers, pharmacists, and care managers, making the most of limited resources. Imagine your own “practice of the future” in which all these access points are available, virtually and in-person, seamlessly integrated, and supporting physician and patient in creating the best possible outcomes. Would that be a compelling value proposition (assuming our competition doesn’t develop it first)?
These are big questions…the type of questions that we’re really good at helping clients solve. If these are keeping you up at night, we invite you to give us a call – we’d love to start a conversation as thinking partners on your journey to “stability and normalcy.”
Related Strategy Resources











